Artificial intelligence is making waves across many fields and diagnostic imaging centers are on the frontline of change. Radiology suites already collect vast amounts of image data and smart algorithms can act like extra sets of eyes that sift through pictures at speed.
Staff face pressure to keep up with demand and still catch subtle signs that human vision might miss, so tools that spot patterns quickly are attractive. The promise of faster reads and clearer prioritization stirs curiosity and cautious optimism among clinicians and patients alike.
How AI Processes Medical Images
Modern AI systems learn from many labeled examples and detect patterns across pixels that human observers might overlook. Training involves feeding the model a large corpus of scans so it can learn what normal and abnormal features look like and then apply that learned mapping to new cases.
These systems use layered computations to extract features from low level edges up to higher level structures and then match those features to likely diagnoses. The result is not a single magic answer but a probabilistic signal that helps prioritize or augment human interpretation.
Improving Image Acquisition And Quality
AI can help techs get better images at the source by suggesting optimal acquisition parameters and flagging motion or exposure issues in real time. Smarter scanners guided by algorithms can reduce repeat scans, shorten exam times, and cut patient discomfort since fewer retakes are needed.
Algorithms can also clean up noisy data and reconstruct higher resolution pictures from limited input, which is handy when scanning fragile patients who cannot stay still. Those improvements translate into clearer pictures for the radiologist and a smoother day for staff and patients.
Enhancing Diagnostic Accuracy And Detection
Pattern recognition systems can spot subtle abnormalities that might be easy to miss, such as tiny nodules or early signs of disease in dense tissue. When AI highlights suspicious regions it can draw attention to findings that merit a second look, helping reduce false negatives while also offering a second opinion on tricky cases.
Over time the human reader and algorithm can form an effective partnership where each compensates for the other s blind spots and the combination yields higher total accuracy. Still, algorithms produce probabilities not certainties, so human judgment remains central.
Streamlining Workflow And Prioritization
Triage tools powered by AI can rank studies by urgency so critical cases reach the top of the reading list without delay. By flagging urgent bleeds or large strokes these systems help clinical teams act faster and allocate resources where they matter most.
Automated report generation can handle routine descriptions and measurements, freeing radiologists to focus on interpretation rather than repetitive text entry.
Some healthcare software providers are also focusing on helping centers automate front-office work, allowing staff to manage scheduling, patient intake, and administrative tasks more efficiently while clinical teams concentrate on diagnosis and care. That time can be used for complex cases, teaching, or direct consultation with referring clinicians.
Integrating With Radiologist Expertise
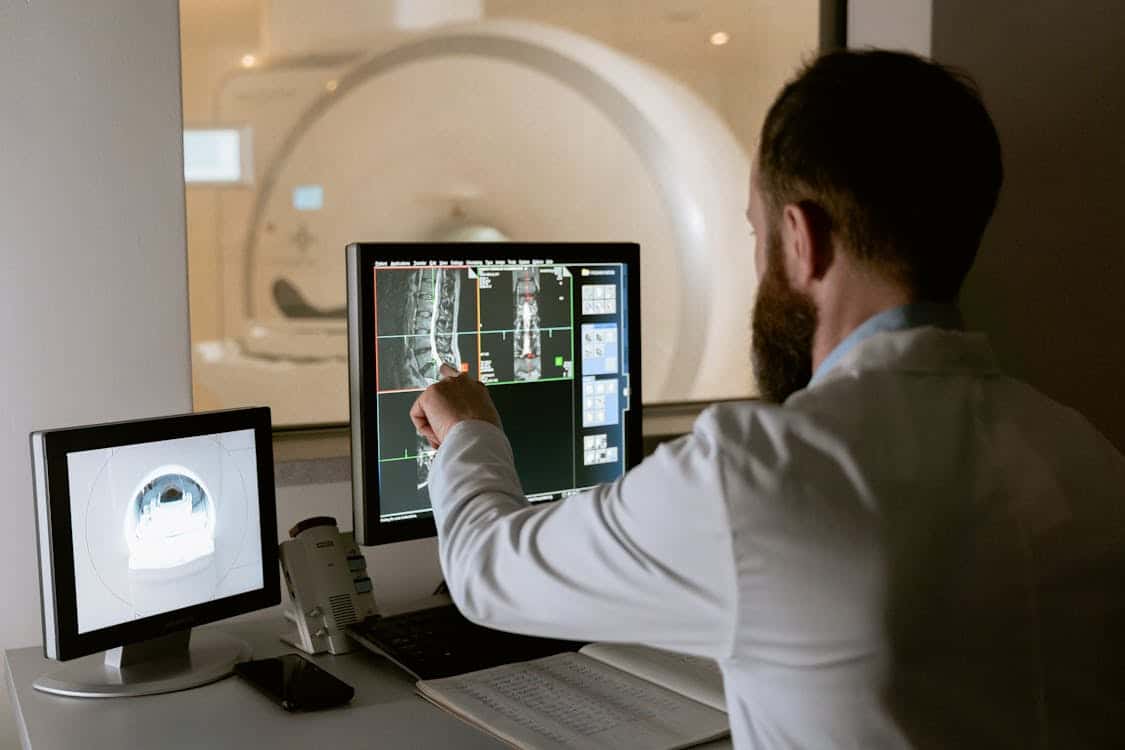
AI works best when it complements the clinician rather than replaces them, creating an environment where experience and algorithmic speed meet. Radiologists retain final responsibility and can use AI output to confirm hunches or explore alternative explanations, treating the tool as a diagnostic colleague rather than an oracle.
Training programs that teach how to interpret algorithmic outputs and spot algorithmic failure modes are key to safe adoption. A healthy skepticism paired with openness to new workflows helps teams reap benefits without blind acceptance.
Data Privacy And Ethical Considerations
Large scale model training requires access to patient images and metadata, which raises privacy and governance questions that must not be ignored. Centers need robust deidentification, secure storage, and clear policies about who can access data and for what purpose.
Transparency about algorithm performance across different patient groups is essential to guard against biased outcomes and unequal care. Patients and staff should be part of the discussion so ethical choices reflect shared values and legal obligations.
Cost And Access Implications
Upfront investment in software, hardware, and staff training represents a real barrier for smaller clinics and rural centers that already operate on thin margins. On the other hand certain platforms promise scalable pricing and cloud based tools that lower the entry point, creating new pathways for underserved locations to gain advanced capabilities.
Return on investment can come from fewer repeat scans, faster throughput, and better resource allocation, though the numbers vary widely by setting. Thoughtful procurement and pilot trials help administrators weigh tradeoffs before committing to broad deployment.
Regulatory And Validation Pathways
Before being relied upon clinically, AI tools must pass through validation studies that test performance against accepted standards and diverse populations. Regulatory clearance offers a baseline of safety but local validation helps teams understand how a tool performs within their unique patient mix and scanner fleet.
Continuous monitoring after deployment catches drift in performance when data distributions shift or new scanner models come online. Clear reporting of false positive and false negative rates helps clinicians calibrate trust and decide how much weight to give algorithmic suggestions.
Training Staff And Fostering Adoption
Successful integration calls for hands on training that lets radiologists and technologists experiment with new workflows without fear of penalties for early mistakes. Peer learning and champions within the department can break resistance to change by showing practical benefits and troubleshooting common issues.
Documentation that explains the limits of any tool and simple checklists for when to override algorithmic output build safer habits. When teams invest time in shared learning they often find the technology becomes an accepted part of everyday practice.
Future Development And Practical Steps For Centers
Incremental deployment through targeted pilots helps teams learn and adapt without overcommitting resources or disrupting care delivery in one big leap. Interoperability with existing picture archiving and communication systems plus robust vendor support smooth the path from testing to routine use.
Ongoing partnerships between clinical teams, engineers, and ethicists help shape tools that solve real problems rather than shiny but impractical features. As real world experience accumulates, imaging centers can refine protocols, create local quality checks, and set realistic expectations about what smart algorithms add to patient care.